Around four percent of fractures affect the clavicle (collar bone), most of these are treated with conservative measures. However, many clavicle fractures benefit from a surgery called open reduction and internal fixation (ORIF).
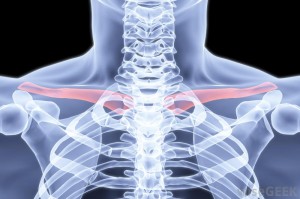
This surgery is done on moderate to severe clavicle fractures. Epidemio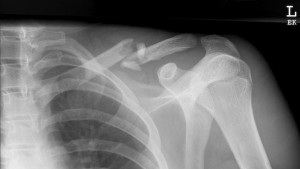 logical studies proved that approximately 80 percent of clavicular fractures occur in the middle third section of the bone, whereas, 15 percent occur in the distal third and only five percent occur in the medial third aspect of the clavicle.
logical studies proved that approximately 80 percent of clavicular fractures occur in the middle third section of the bone, whereas, 15 percent occur in the distal third and only five percent occur in the medial third aspect of the clavicle.
Non-operative treatment of clavicular fractures can lead to a deformity of the shoulder and difficulty with joint function. Many reports regarding complication rates of displaced clavicle fractures in adult patients show that outcomes are much less satisfactory than for younger people.
Malunion or nonunion of the clavicle pieces lead to several issues, such as deformity, pain, weakness, decreased function, and neurovascular symptoms. There is increasing recognition of poor outcomes following these fractures that have led to a renewed interest in internal fixation of an adult displaced fracture of the clavicle.
When assessing a patient with a clavicular fracture, the upper arm is 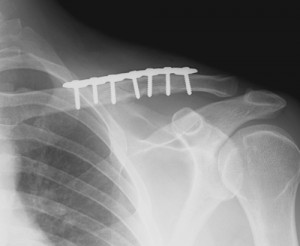 evaluated for evidence of vascular compromise by comparing peripheral pulses, color, temperature, and blood pressure of the injured extremity with the other extremity. When the comparison yields no deviations or variances, an angiogram is not necessary. Angiogram evaluation is done to assess for vascular injury only, and in high-energy impact trauma patients, x-rays of the chest are done to assess for rib fractures and pneumothorax.
evaluated for evidence of vascular compromise by comparing peripheral pulses, color, temperature, and blood pressure of the injured extremity with the other extremity. When the comparison yields no deviations or variances, an angiogram is not necessary. Angiogram evaluation is done to assess for vascular injury only, and in high-energy impact trauma patients, x-rays of the chest are done to assess for rib fractures and pneumothorax.
Indications for a clavicle fracture surgery include:
- High level athlete who wants to get back on the field faster.
- Associated vascular injury
- Open fracture
- Progressive neurological deficits
- Torn coracoclavicular ligaments with distal fracture
- Serious medialization of the shoulder girdle
- Gross displacement that can lead to skin breakdown
- Multiple injuries
- Torn coracoclavicular ligaments with distal fractures
ORIF Surgical Technique
The ORIF surgery is performed under general anesthesia, and Beverly Hills orthopedic surgeons often use a regional nerve block along with it to boost postoperative pain control.
The patient is operated on in the beach-chair position. An incision is made over the center of the fracture site, and the subcutaneous tissue is raised as a flap, with the underlying myofasica reflected upward. After the ends of the fracture are fixed with plates, wires, and/or screws, the incision is sutured and a dry sterile bandage is applied.
 The patient is moved to a recovery room for stabilization. Once stable, most patients can be discharged to home with the operative side immobilized in a sling or shoulder immobilizer.
The patient is moved to a recovery room for stabilization. Once stable, most patients can be discharged to home with the operative side immobilized in a sling or shoulder immobilizer.
Pendulum exercises are done during the first postoperative week, with active-assisted motion done at two weeks. This allows the patient to improve function and restore independence to do activities of daily living. Additionally, sutures are removed in 10 to 14 days following surgery.
The orthopedic specialist in Los Angeles will have the patient return for follow-ups at two to four week intervals during the first couple of months after the ORIF procedure. Standard x-rays are done to visualize the hardware and assess fracture healing. When there is no loss of reduction on x-rays, the physical therapist begins strengthening activities and active and passive range of motion.
Dr. Raj is a top Beverly Hills Orthopedic Surgeon, and offers treatment for all types of orthopedic conditions including collar bone fractures. Dr. Raj is Double Board Certified, and provides operative and nonoperative treatments including:
- Pain Medications
- Bracing
- Stem Cell therapy
- Surgical Fixation