Joint replacement surgeries, especially those of the lower extremities, are becoming increasingly more common today. One of the major risk factors associated with this type of surgery is a postoperative complication known as deep vein thrombosis (DVT). 
A DVT is the formation of a blood clot (embolus) within a deep vein, and this typically occurs in either the calf or thigh. While DVT can develop after any kind of major surgery, patients who undergo lower extremity surgeries are particularly vulnerable.
Following hip surgery, thrombi (enzymes that facilitate the formation of clots) often develop in the thigh veins. These clots are more likely to lead to pulmonary embolism (PE) than those that form deep within the calf following a knee procedure. While clots in the calf are less likely to lead to PE, they can be harder to detect.
Prevention of Blood Clots
Blood clot prevention is an approach used by Los Angeles orthopedic surgeons to specifically address coagulation and stasis issues. Generally, they utilize several therapies in combination. Patients will likely be fitted with elastic compression stockings, as well as an external compression device, when they are initially admitted to hospital.
 Movement and rehabilitation exercises commence on the first postoperative day, typically continuing for several months following surgery. In addition, anticoagulant therapy usually begins the night before the surgical procedure, continuing for a prescribed period at home.
Movement and rehabilitation exercises commence on the first postoperative day, typically continuing for several months following surgery. In addition, anticoagulant therapy usually begins the night before the surgical procedure, continuing for a prescribed period at home.
Early Movement and Rehabilitation
Rehabilitation and early movement are both beneficial and critical after surgeries on the lower extremities. Physiotherapy such as range of motion of the joint(s), isotonic and isometric exercises, and gait training all generally start on the first postoperative day.
Mechanical Prevention
Mechanical preventions, utilized in combination with other therapies, often include the following:
- Exercises (simple leg lifts), elevating the bottom of the bed, and active/passive ankle motion to increase blood flow throughout the femoral vein.
- Compression stockings are used following both hip and knee replacements. However, they appear to be more effective in preventing the formation of clots within the calf than within the thigh.
- External pneumatic compression devices, which apply pulsating pressure much like what actually takes place during normal walking, can assist in the overall reduction of DVT. They are utilized along with other therapies. These devices can be difficult to apply often making patient compliance an issue.
Drug Prevention
The risk of the formation of deep vein thrombosis is the greatest in the first two to five day period following surgery. Most commonly administered anticoagulants used to prevent the occurrence are aspirin, Coumadin (warfarin), and heparin.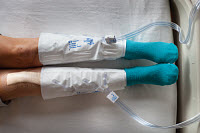
Aspirin (ASA)
ASA is very easy to give and costs very little and it possesses very few bleeding complications. It does not need to be monitored as closely as other medications but ASA has not been proven to be more effective than other drugs, so it may not be recommended for all joint replacement patients. Research has shown that aspirin does have a greater protective effect on PE in men.
Coumadin (Warfarin)
Coumadin, the most commonly used anticoagulant for knee and hip replacement patients, disrupts the metabolism of vitamin K within the liver to prevent certain clotting factors from forming. This particular medication takes a minimum of 36 hours to take effect and between four and five days to reach its maximum efficacy. Hence, Coumadin therapy is often started the day before surgery is scheduled. Low doses are administered since higher doses can precipitate bleeding episodes.
Heparin
Heparin, a natural substance inhibiting the clotting mechanism, is effective following both knee and hip replacement  procedures. However, there is an increased bleeding risk when it is administered following knee replacements. Since heparin works more quickly than coumadin does, it is often given at first then followed by coumadin therapy or heparin can also be used as a single agent.
procedures. However, there is an increased bleeding risk when it is administered following knee replacements. Since heparin works more quickly than coumadin does, it is often given at first then followed by coumadin therapy or heparin can also be used as a single agent.

